The degree of neuromuscular block can be assessed by applying a supramaximal stimulus to a peripheral nerve, and then measuring the associated muscular response. (The motor unit consists of a motor neurone and a muscle, which are separated by the neuromuscular junction.
How do you assess neuromuscular function?
The most reliable method of measuring neuromuscular function is to stimulate an accessible peripheral motor nerve and measurement of the evoked response of the skeletal muscle or muscles innervated by the stimulated motor nerve.
What is physical manifestation of neuromuscular blockade?
After a period of rapid stimulation (tetany), the nerve cells gear up for action. After a brief pause, the twitch height will be increased above baseline for that degree of block. Not only the height, but the number of twitches increases.
What is used to assess neuromuscular?
Objective evaluation involves recording, processing, and measuring muscle responses to nerve stimulation. Ideally, when neuromuscular-blocking drugs are used, the neuromuscular function should be monitored with the use of quantitative means, including acceleromyography, kinemyography, and electromyography.What is the most sensitive indicator of recovery from neuromuscular blockade?
7 In clinical use, it is easier for clinicians to assess fade with double burst stimulation vs TOF, but 100-Hz tetanus over 5 seconds appears to be the most sensitive test for assessing RNMB.
How is neuromuscular transmission measured?
How is the NMT block measured? The level of neuromuscular block is routinely measured by stimulating a peripheral nerve, usually in the hand and by subjectively evaluating the muscle response either visually or tactilely with a device.
What is quantitative neuromuscular monitoring?
Quantitative monitoring uses neuromuscular monitors, devices that stimulate the peripheral nerve while also recording, quantifying and displaying numerically the evoked responses [21]. Multiple techniques are in use, for which we presented advantages and limitations in Table 1.
Which nerve is tested for adequacy of Anaesthesia?
Measurement of the tension in the adductor pollicis muscle after electrical stimulation of the ulnar nerve is an established technique in human muscle physiology and widely used in anesthesia [1,2]. The accepted method of stimulating the adductor pollicis involves placing electrodes at the wrist over the ulnar nerve.What is neuromuscular junction and its function?
The neuromuscular junction (NMJ) is a highly specialized synapse between a motor neuron nerve terminal and its muscle fiber that are responsible for converting electrical impulses generated by the motor neuron into electrical activity in the muscle fibers.
How do paralytic drugs work?Paralytic drugs temporarily interfere with the messages that nerves send to the skeletal muscles of the body. The skeletal muscles are those that control movements of the face, arms, legs, back, and trunk. The muscles of the diaphragm, which help expand the lungs, are also paralyzed by these medications.
Article first time published onWhat type of drug is rocuronium?
Rocuronium is a non-depolarizing neuromuscular blocker widely used to produce muscle relaxation to help facilitate surgery and ventilation of the lungs in elective and emergent situations.
What nursing intervention should be included in the nursing management of the patient receiving a neuromuscular blocking agent?
Ensure patient is fully ventilated on a controlled rate of breathing before administration of a Neuromuscular Blocker (NMB). Patient requires an arterial line and End Tidal CO2 Monitoring. Ensure ECG, oxygen saturation, End Tidal CO2 and arterial pressure alarms are on with appropriate alarm settings.
How do you assess a train of four?
Turn on the peripheral nerve stimulator and select a low amplitude, usually 10 or 20 mA to start. Increase the current in increments of 10 mA until 4 twitches are observed. Note the current (in mA) that corresponds to 4 vigorous twitches when the train-of-four stimuli button is pushed.
What is BIS monitoring in ICU?
Bispectral index (BIS) monitoring, an objective measure of the patient’s response to sedation, has been used in anesthesia for over a decade. This technology is finding its way into the ICU to provide a means of assessing the adequacy of sedation and preventing oversedation of critically ill patients.
How often should train of four be assessed?
If patient remains at the TOF goal and clinical goal, assess TO4 at least every 4 hours while on continuous NMBA.
Why is there no fade with succinylcholine?
The resultant end plate depolarization initially stimulates muscle contraction; however, because succinylcholine is not degraded by acetylcholinesterase, it remains in the neuromuscular junction to cause continuous end plate depolarization and subsequent muscle relaxation. This is termed a phase I block.
How common is residual neuromuscular blockade?
Discussion. Residual neuromuscular block is commonly observed postoperatively in patients administered NMBAs. Studies have demonstrated that approximately 40% of patients administered intermediate-acting NMBAs have TOF ratios less than 0.9 in the PACU.
What is qualitative monitoring?
Qualitative monitoring and evaluation methods involve collecting and analysing data in the form of words rather than numbers. … Qualitative monitoring and evaluation (M&E) methods involve collecting and analysing data in the form of words rather than numbers.
How do you count post Tetanic?
It consists of applying a 50-Hz tetanic stimulus to the ulnar nerve for 5 s, followed by single twitch stimulation at 1 Hz. The number of twitches observed in the period of post-tetanic facilitation, the post-tetanic count, correlates inversely with the degree of neuro- muscular blockade.
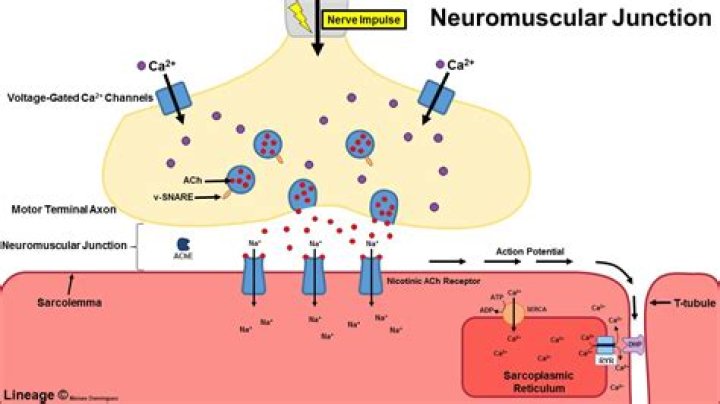
What are the steps of neuromuscular transmission?
Neuromuscular transmission is dependent on a coordinated mechanism involving (1) synthesis, storage, and release of acetylcholine from the presynaptic motor nerve endings at the neuromuscular junction; (2) binding of acetylcholine to nicotinic receptors on the postsynaptic region of the muscle membrane, with consequent …
What is a neuromuscular junction test?
Rather than relying on the subject’s voluntary muscle contractions, they involve activating the NMJ with repeated electrical stimulation of a motor nerve and measuring the size of the summated electrical response of the excited muscle fibres (the compound muscle action potential or CMAP).
What is a single fiber EMG test?
Single-fiber electromyography (SFEMG) is a selective EMG recording technique that allows identification of action potentials (APs) from individual muscle fibers.
What are the 3 components of neuromuscular junction?
For convenience and understanding, the structure of NMJ can be divided into three main parts: a presynaptic part (nerve terminal), the postsynaptic part (motor endplate), and an area between the nerve terminal and motor endplate (synaptic cleft).
What are the three components of the neuromuscular junction?
The neuromuscular junction (NMJ; AKA myoneural junction or motor end-plate) is the synapse between the nerve and muscle. It has three basic components: 1) presynaptic motor nerve terminal, 2) synaptic space (synaptic cleft), and 3) the postsynaptic surface of the skeletal muscle fiber.
How are signals transmitted across the neuromuscular junction?
Acetylcholine is a small molecule that acts as a chemical messenger to propagate nerve impulses across the neuromuscular junction between a nerve and a muscle. When the nerve impulse from a motor neuron arrives at the tip of its axon, acetylcholine molecules stored there in vesicles are released into the synaptic gap.
What is BIS in medical terms?
Article Content. A bispectral index (BIS) monitor is commonly utilized to assess depth of sedation when administering sedative, hypnotic, or anesthetic agents during surgical and medical procedures. The depth of sedation is calculated by measuring cerebral electric activity via an electroencephalogram (EEG).
Is propofol a paralytic drug?
Propofol is given in doses of 0.5 mg/kg to 2 mg/kg intravenously, depending on hemodynamic stability. Immediately after the induction agent, the paralytic agent of choice is administered intravenously.
When do you use paralytics?
Managing physicians should not use paralytics in all cases; rather, they should use them only in those where length of ventilation is expected to exceed a few hours. Patients should not remain ventilated for longer than it takes for the paralytics to have their effect.
How long does it take a paralytic to work?
Paralysis is preceded by a brief period of intense muscle fasiculation and rigidity. The drug is rapidly metabolized by plasma cholinesterase, which results in a duration of effect of 5 to 10 minutes following a standard dose.
What is propofol used for?
Propofol injection is used to help you relax or sleep before and during surgery or other medical procedures. This medicine is an anesthetic and a sedative. Propofol may also be used to sedate coronavirus (COVID-19) patients who need mechanical ventilation in the intensive care unit (ICU).
Does rocuronium stop breathing?
It works by blocking the signals between your nerves and your muscles. Rocuronium is given before general anesthesia in preparing you for surgery. Rocuronium helps to keep your body still during surgery. It also relaxes your throat so a breathing tube can be more easily inserted before the surgery.