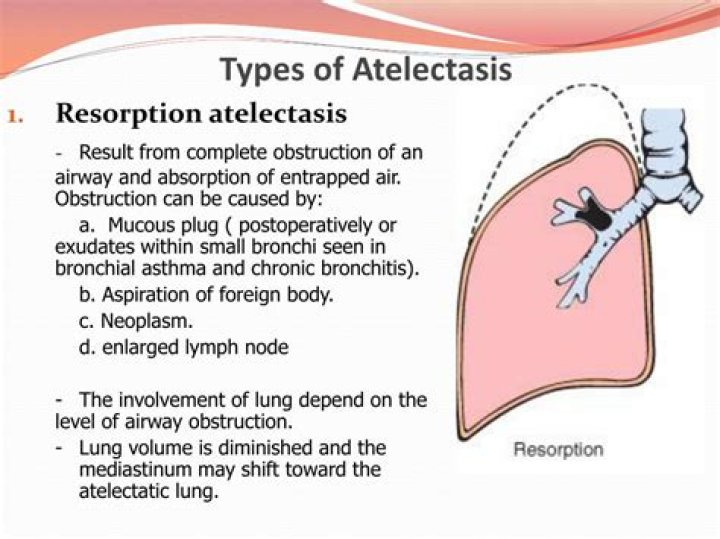
Resorption atelectasis is the most common mechanism of volume loss and results from obstruction in airflow somewhere between the trachea and the alveoli.
What is reabsorption atelectasis?
Resorptive or obstructive atelectasis is a form of lung collapse that is due to obstruction of the airways supplying a lung segment or lobe. It is a term used to distinguish atelectasis identified on imaging based on the underlying pathophysiology to guide diagnosis.
What are the signs of absorption atelectasis?
- Trouble breathing (shortness of breath)
- Increased heart rate.
- Coughing.
- Chest pain.
- Skin and lips turning blue.
What causes resorption atelectasis?
Resorption atelectasis is caused by resorption of alveolar air distal to obstructing lesions of the airways; adhesive atelectasis stems from surfactant deficiency; passive atelectasis is caused by simple pneumothorax, diaphragmatic dysfunction, or hypoventilation; compressive atelectasis is due to tension pneumothorax, …How long does it take for absorption atelectasis to occur?
At FiO2 of 0.3, atelectasis takes hours to develop secondary to absorption; however, this is reduced to approximately 8 minutes with an FiO2 of 1.0. Also, small airways may become completely occluded causing distal gas to be trapped and absorbed leading to airway collapse.
Should I worry about atelectasis?
In an adult, atelectasis in a small area of the lung is usually not life threatening. The rest of the lung can make up for the collapsed area, bringing in enough oxygen for the body to function.
How do you stop atelectasis absorption?
How can you reduce the risk of absorption atelectasis? Preventing absorption atelectasis begins by addressing any potentially problematic respiratory conditions before a surgical procedure, including advising individuals to stop smoking in the weeks prior to surgery.
Does oxygen help atelectasis?
Ventilation of the lungs with pure oxygen after a vital capacity manoeuvre that had re-opened a previously collapsed lung tissue results in rapid reappearance of atelectasis. If 40% O2 in nitrogen is used for ventilation of the lungs, atelectasis reappears slowly.Which type of atelectasis is the most common?
Obstructive atelectasis is the most common type and results from reabsorption of gas from the alveoli when communication between the alveoli and the trachea is obstructed. The obstruction can occur at the level of the larger or smaller bronchus.
What is the most common cause of lobar atelectasis?Lobar atelectasis occurs in a variety of medical conditions, such as a critical illness, a postoperative complication, a trauma, or lung cancer. The main etiology of lobar atelectasis is bronchial obstruction by mucus plugs from buildup of copious purulent secretions due to defective clearance mechanisms.
Article first time published onIs Bibasilar atelectasis serious?
The complications of bibasilar atelectasis can become serious if not treated by your doctor or a medical professional. The following are some possible complications of bibasilar atelectasis: Hypoxemia. This is when there are low oxygen levels in your blood.
What is the treatment for Subsegmental atelectasis?
Atelectasis treatments include: Bronchoscopy to clear blockages like mucus. Medicine that you breathe in through an inhaler. Physiotherapy such as tapping on your chest to break up mucus, lying on one side or with your head lower than your chest to drain mucus, and exercises to help you breathe better.
Can atelectasis go away?
Treatment of atelectasis depends on the cause. Mild atelectasis may go away without treatment. Sometimes, medications are used to loosen and thin mucus. If the condition is due to a blockage, surgery or other treatments may be needed.
How do you fix atelectasis?
Atelectasis treatment can include breathing or coughing exercises, inhaled medicines, breathing devices, or surgery. Atelectasis usually gets better with time or treatment. However, if it is undiagnosed or untreated, serious complications can occur, including fluid buildup, pneumonia, and respiratory failure.
Can too much oxygen cause atelectasis?
Oxygen toxicity can cause a variety of complications affecting multiple organ systems. CNS complications primarily include tonic-clonic convulsions and amnesia. Pulmonary sequelae range from mild tracheobronchitis and absorptive atelectasis to diffuse alveolar damage that is indistinguishable from ARDS.
What's the difference between lung collapse and atelectasis?
A collapsed lung happens when air enters the pleural space, the area between the lung and the chest wall. If it is a total collapse, it is called pneumothorax. If only part of the lung is affected, it is called atelectasis.
What is the difference between absorption atelectasis and compression atelectasis?
Compression atelectasis occurs when the transmural pressure distending the alveolus is reduced. Absorption atelectasis occurs when less gas enters the alveolus than is removed by uptake by the blood.
What may help prevent atelectasis in the operating room?
Clinical implications The findings in the current study indicate that a moderate PEEP alone may be sufficient to maintain oxygenation and nearly prevent atelectasis in a vast majority of normal-weight, healthy patients undergoing low-risk surgery.
How does atelectasis cause positive pressure ventilation?
During mechanical ventilation (positive pressure ventilation), atelectasis may occur when lungs are underinflated due to low tidal volumes, or when compression occurs (such as patient position or obesity).
Can atelectasis cause back pain?
Symptoms of Atelectasis and Pneumothorax Sudden, sharp pain in the chest or radiating to the shoulder or back.
What are the 3 types of atelectasis?
There are three major types of atelectasis: adhesive, compressive, and obstructive.
What does atelectasis mean in medical terms?
Atelectasis (at-uh-LEK-tuh-sis) is a complete or partial collapse of the entire lung or area (lobe) of the lung. It occurs when the tiny air sacs (alveoli) within the lung become deflated or possibly filled with alveolar fluid. Atelectasis is one of the most common breathing (respiratory) complications after surgery.
What lung sounds do you hear with atelectasis?
- atelectasis,
- congestive heart failure (CHF), or.
- pulmonary fibrosis.
Does Covid 19 cause atelectasis?
Previous studies reported a lower incidence of atelectasis in patients with COVID-19 pneumonia [3]. Our data suggest that the presence of large atelectasis may be a factor affecting progressive evolution to the ARDS [16].
What does it feel like to have a partially collapsed lung?
A collapsed lung feels like a sharp, stabbing chest pain that worsens on breathing or with deep inspiration. This is referred to as “pleuritic” because it comes from irritation of nerve endings in the pleura (inner lining of the rib wall).
Can you have a partially collapsed lung and not know it?
It is possible to have a partial or complete lung collapse. Sometimes a partial collapse might affect just a small part of the lung, and you may only have mild symptoms, or may even feel nothing.
Can atelectasis cause dizziness?
Shortness of breath. Chest pain that is worse with breathing. Dizziness, weakness, or fainting. Coughing up blood.