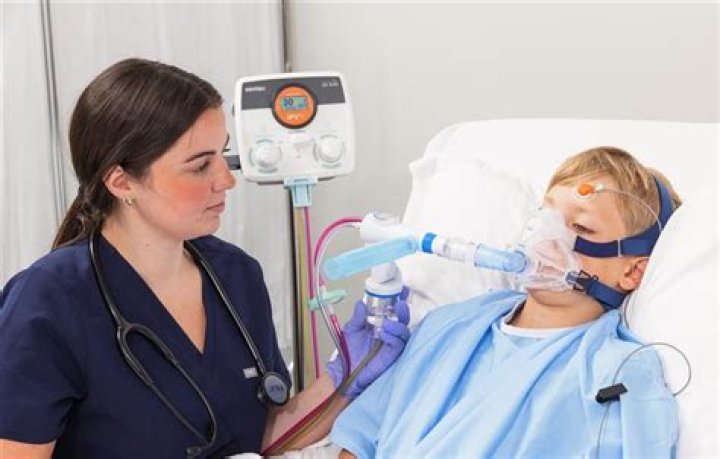
Intrapulmonary percussive ventilation (IPV) is a form of chest physical therapy administered to the airways by a pneumatic device. Using a breathing circuit called a Phasitron, mini bursts of gas are delivered into the lungs at rates between 100 – 300 breaths per minute (bpm).
How are the lungs protected from barotrauma with the IPV?
IPV was designed to improve mucus clearance and recruit obstructed bronchi and alveoli using a lung protective strategy; it avoids barotrauma caused by over-inflation of preferential airways. By improving mucus clearance, hyperinflation is reduced, and lung mechanics and gas exchange are improved (1).
How long is IPV treatment?
Instructions to Perform IPV Treatment Each cycle lasts for five minutes and has its own settings.
What is a VDR ventilator?
The Volumetric Diffusive Respirator unit (VDR®-4) is a flow-regulated and time-cycled ventilator that provides high-frequency percussive ventilation (HFPV).How do you do PEP therapy?
Instructions to Use PEP Have your child hold their breath for two to three seconds. Have your child breathe out through the mask into the PEP device to create pressure 10-20 cm H2O. Have him / her breathe out for four to six seconds until just beyond a normal breath. Repeat 15 times (one cycle).
How does a jet ventilator work?
In HFJV a jet is applied with a set driving pressure, followed by passive exhalation for a very short period before the next jet is delivered, creating “auto-PEEP” (called pause pressure by the jet ventilator). The risk of excessive breath-stacking leading to barotrauma and pneumothorax is low but not zero.
What is the difference between an oscillator and ventilator?
High-frequency oscillation (HFO) ventilation differs from conventional ventilation in that very small breaths are delivered very rapidly (180 to 900 breaths per minute). HFO helps with the opening of collapsed lung tissue by providing constant positive pressure in a person’s airway.
What are the contraindications for IPV?
Poliovirus vaccine, inactivated, IPV is contraindicated for use in patients who have experienced anaphylaxis or anaphylactic shock within 24 hours of a previous dose of the vaccine or any of its components, as well as patients with streptomycin hypersensitivity, neomycin hypersensitivity, polymyxin hypersensitivity, …How often should an IPV screening be done?
It is best practice for all home visiting programs to screen primary caregivers for IPV at least once per year. The HARK is a four question, self-reported screening tool that represents different components of IPV including emotional, sexual, and physical abuse.
How does a Phasitron work?The Phasitron® is a unique venturi that acts as a “clutch” mechanism to protect the lung from over pressure. By automatically adjusting to the resistance of the lung, the Phasitron® precisely and safely delivers the optimal volume and pressure of air required by the alveolar space.
Article first time published onWhat is the best PEP device?
The Aerobika produced the greatest peak PEP overall at medium and high resistance, and the Pari PEP S produced the lowest peak PEP overall at low and medium resistance.
When is PEP used?
What is PEP. PEP (sometimes called PEPSE) is a combination of HIV drugs that can stop the virus taking hold. It can be used after the event if you’ve been at risk of HIV transmission. To work, PEP must be taken within 72 hours (three days), and ideally should be taken within 24 hours.
What are the indications for PEP therapy?
Three common indications for PEP are to increase lung volume (Functional Residual Capacity (FRC) and Tidal Volume (VT)), to reduce hyperinflation and to improve airway clearance [12], [13], [14].
What is a chest wiggle?
Chest wiggle: The body wiggle or vibration caused by HFV. Power: The electrical current control that displaces the diaphragm-sealed piston; as the piston is displaced in a forward and backward square-wave pattern, amplitude fluctuations are superimposed. Tidal volume (VT): Volume of gas for each breath.
What is neonatal Hfov?
High-frequency oscillatory ventilation (HFOV) is a lung-protective strategy that can be utilized in the full spectrum of patient populations ranging from neonatal to adults with acute lung injury. HFOV is often utilized as a rescue strategy when conventional mechanical ventilation (CV) has failed.
What is an oscillator in the NICU?
Unlike traditional ventilators, which essentially inflate and deflate the baby’s lungs like a set of billows, the oscillator keeps the lungs open with a constant positive end-expiratiory pressure (“PEEP”) and vibrates the air at a very high rate (up to 600 times per second).
What is a normal PIP on ventilator?
PIP: Total inspiratory work by vent; Reflects resistance & compliance; Normal ~20 cmH20 (@8cc/kg and adult ETT); Resp failure 30-40 (low VT use); Concern if >40. Pplat-PEEP: tidal stress (lung injury & mortality risk). Target < 15 cmH2O.
Why do Jets have ventilation?
Jet ventilation is an effective alternative mode of ventilation that achieves alkalization at lower mean airway pressures and significantly improves cardiac output (Dietrich et al., 1993).
What are the two types of medical ventilation?
- Positive-pressure ventilation: pushes the air into the lungs.
- Negative-pressure ventilation: sucks the air into the lungs by making the chest expand and contract.
How do you detect IPV?
Several screening instruments can be used to screen women for IPV in the past year, such as the following: Humiliation, Afraid, Rape, Kick (HARK); Hurt/Insult/Threaten/Scream (HITS); Extended–Hurt/Insult/Threaten/Scream (E-HITS); Partner Violence Screen (PVS); and Woman Abuse Screening Tool (WAST).
What is the most widely used IPV screen?
The most studied IPV screening tools were the Hurt, Insult, Threaten, and Scream (HITS),13–15,24,43 the Woman Abuse Screening Tool/Woman Abuse Screening Tool-Short Form (WAST/WAST-SF),15–17,25,26,44 the Partner Violence Screen (PVS),22–26,44 and the AAS.
Which finding is common among victims of intimate partner violence IPV )?
The most common physical symptoms include injuries, headaches, insomnia, chronic pain, choking sensations, hyperventilation, and gastrointestinal symptoms, chest, back, and pelvic pain. IPV can also result in unplanned pregnancies and pregnancy complications for the mother and child.
How do you administer IPV?
Single-antigen IPV (IPOL) is distributed in single-dose syringes or in 10-dose vials. The recommended dose for both children and adults is 0.5 mL. It can be administered by the intramuscular or subcutaneous route, using a needle length appropriate for the age and size of the person receiving the vaccine.
Who should not get the inactivated polio vaccine?
Hypersensitivity or Anaphylactic Reactions People who have had severe allergic (anaphylactic) reactions after a previous dose of inactivated polio vaccine (IPV) or after taking streptomycin, polymyxin B, or neomycin should not receive IPV.
When should not give polio drops?
Use of OPV is not recommended in neonates less than 6 weeks of age. Poliomyelitis has occurred after OPV administration both in vaccinees and in their close contacts. Poliovirus may be shed in the feces (and possibly from the pharynx) of vaccinees for 6-8 weeks after OPV administration.
What is IPV pulmonary?
Intrapulmonary percussive ventilation (IPV) derives from high-frequency percussive ventilation, which was initially applied to treat respiratory failure after smoke inhalation or burns. 8–11. It is a pressure-limited, time-cycled, high-frequency mode of ventilation that delivers sub-physiologic tidal volumes.
What is MetaNeb therapy?
The MetaNeb® System is designed to mobilize retained secretions, lung expansion therapy, and to deliver medicated aerosol for the treatment and prevention of pulmonary atelectasis. It also has the ability to provide supplemental oxygen when used with compressed oxygen.
What is Ezpap?
Portex® The EZPAP® positive airway pressure system is used to expand the lungs by increasing Functional Residue Capacity (FRC). Increasing FRC has been found to contribute to the prevention and reversal of atelectasis.
Can you get PEP from a pharmacy?
You can buy the emergency contraceptive pill from chemists, and it is usually also available from GPs, sexual health clinics and A&E departments.
What is PEP physiotherapy?
Positive expiratory pressure (PEP) therapy involves breathing with a slightly active expiration against an expiratory resistance. It is used for: clearance of excess secretions from the lungs. reducing gas trapping and improving ventilation of the lungs.
How much does PEP treatment cost?
How much does PEP cost? A complete course of PEP can cost from $597 to $1,000 without insurance. However, most insurance providers will cover PEP. In some cases, an individual may not need to pay for PEP.